Quick Summary
Traditional credentialing takes 60 to 120 days. Every idle provider is just lost revenue. We evaluated eight platforms on execution speed, first-pass approval rates, automation depth, and enrollment capabilities. Here are our top three picks:
Why Listen to Us
We built Assured after scaling a provider network from 0 to 150+ providers across 15 states and living every credentialing bottleneck firsthand. Today, we’re an NCQA-certified CVO serving health systems and digital health organizations nationwide, so we know this space: the vendors, the gaps, and what actually works.
Why Choosing a Good Credentialing Software Is Important?
For most of healthcare's history, credentialing was managed by one or two specialists at a practice who tracked everything in spreadsheets, accessed CAQH manually, and followed up with verification sources by phone and email. This worked (slowly) when practices were small, and provider turnover was low.
Today, three things have converged to break that model.
Growth velocity has accelerated.
Private equity-backed physician groups, digital health companies scaling telehealth, and multi-site pediatric or specialty practices are now onboarding 30 to 50 new providers per year.
In our conversation with a COO building a pediatric network in middle Tennessee, the calculation was explicit: at their growth rate, a single credentialing specialist handling 75 active providers would be overwhelmed within 18 months. The spreadsheet model doesn't scale past a certain inflection point. It just gets louder and more error-prone.
Compliance requirements have also tightened
NCQA and Joint Commission standards require ongoing exclusion monitoring, documented primary source verification, and clear credentialing committee records.
Practices pursuing delegated credentialing must demonstrate months of clean, auditable credentialing activity before a payer will grant that authority. Many payers require a six to twelve-month lookback period of consistent credentialing records. Software that centralizes verification data and produces audit-ready documentation becomes critical in those situations.
The downstream financial impact is also significant
Every day a provider sits credentialed but not enrolled is lost revenue. At typical physician billing rates, even a two-week delay can amount to tens of thousands of dollars. Across a practice adding 40 new providers a year, the math becomes a compelling business case.
The 8 Best Credentialing Software Platforms in 2026
1. Assured
Best for: Growth-stage organizations and enterprises needing credentialing, enrollment, and licensing executed end-to-end
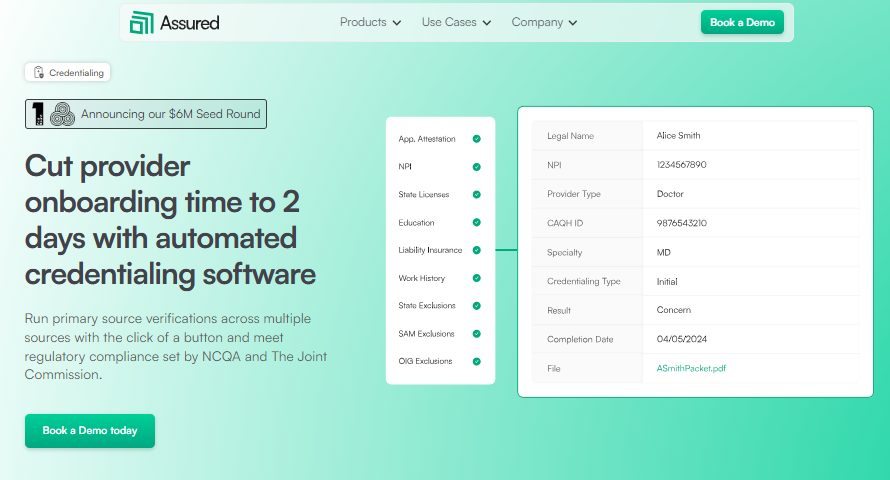
Assured is an AI-powered credentialing platform for healthcare organizations that need to credential providers fast, stay continuously compliant, and scale without adding headcount. It handles the full credentialing lifecycle:
- Data collection from CAQH, NPPES, DEA, and state boards
- Automated parallel PSV across 2,000+ sources;
- NCQA-compliant file generation; ongoing monitoring
- and expirables management
… all in one system.
We're NCQA-certified across all 11 verification elements, and have processed tens of thousands of files for 300+ customers, including Houston Methodist, Tono Health, and Blossom Health.
The difference between Assured and most platforms in this category comes down to one thing: we built software to run the credentialing process fast and smoothly. But how fast? Good question.
We credential providers in 48 hours on average. The industry standard is 60 to 120 days. That gap exists because our PSV engine verifies credentials across 2,000+ primary sources in parallel, not one database at a time. A provider who joins your practice on Monday can have a complete, committee-ready credentialing file by Wednesday.
Accuracy is another big thing for us. Our AI validates every application before it leaves the platform, whether that's a credentialing packet or a payer enrollment submission. That means catching data mismatches, missing documents, and compliance gaps before they become rejection letters or delayed contracts.
Bryson Tombridge, founder of Tono Health, spent two years with a legacy vendor and got zero contracts completed. That delay cost the business an estimated $1 million to $1.5 million. In their first month with us, we completed 120 contracts.
As Bryson put it, “Just shortening the amount of time it takes to get our doctors licensed and credentialed unlocks over $500,000 per provider.” Check out the full case study here.
Key Features
- Automated PSV: Verifications run across 2,000+ primary sources in parallel, cutting credentialing files to as little as 48 hours
- CAQH sync: Daily integration catches profile drift, lapsed attestations, and password mismatches before they create revalidation failures
- Pre-submission validation: Flags data mismatches, missing documents, and specialty conflicts before a credentialing file leaves the platform, supporting 95%+ first-pass approval rates
- Parallel processing: Multiple credentialing applications processed simultaneously, eliminating sequential queue bottlenecks during high-volume onboarding periods
- Expirables monitoring: Continuous checks across OIG, SAM, NPDB, DEA, and all state boards; sanctions flagged within 24 hours; renewals initiated automatically 60 days before expiration
- Delegated credentialing support: Committee file generation, NCQA-aligned documentation, and full audit trails
- Role-based access controls: Granular admin settings so teams control exactly what each user. including providers themselves , can view and edit
- Roster management and update: Centralizes your provider roster with real-time updates across credentialing, enrollment, and compliance.
- All-in-one platform for credentialing, enrollment, data monitoring, and license renewals: Combines all workflows in one system for full visibility from onboarding to ongoing compliance.
Pricing
Custom, based on volume, scope, and which modules you need. Reach out at withassured.com/demo for a tailored quote.
Pros
- Fastest published credentialing turnaround in the category
- All fulfillment staff are direct employees, not third-party BPOs
- Usage-based pricing scales with growth
Cons
- Newer to market than legacy incumbents
2. MedTrainer
Best for: Clinics, FQHCs, and multi-site organizations wanting credentialing and compliance training in one system
MedTrainer is a healthcare workforce compliance platform that combines credentialing, compliance training, policy management, and incident reporting in a single natively built system.
If you need credentialing software alongside compliance training and workforce education (ambulatory surgery centers, community health centers), the combined platform reduces the number of vendor relationships and creates data continuity between credentialing status and compliance requirements.
The platform provides software for your team, with optional managed credentialing for organizations with 10+ providers.
Key Features
- Credentialing management: Automate credentialing including PSV, and license tracking
- Learning management system: Access healthcare-specific courses for training and compliance
- Compliance oversight: Centralize policy management, incident reporting, and safety documentation
- Exclusion monitoring: Screen providers across databases including OIG, LEIE, and SAM
Pricing
Tiered subscription pricing depending on modules and access level.
Pros
- Only platform combining credentialing, LMS, and compliance in one system
- Strong user ratings regarding ease-of-use and tracking
- Responsive support team
Cons
- Not a fully managed services model
- Some users report occasional system slowness
- Limited customization in certain modules
3. Andros

Best for: Health plans, large provider networks, and organizations that treat network development as a strategic function alongside credentialing
Andros is a provider network management and credentialing platform built primarily for health plans and larger telehealth organizations. It combines network lifecycle management — recruiting, contracting, credentialing, and monitoring — under one platform with a repository covering over 8 million providers.
Where Andros stands out is in delegated credentialing and network development at scale. Its data-matching algorithms automate PSV, and the company claims two out of three applications in its system complete without any direct provider input, reducing administrative burden during onboarding. Andros holds NCQA CVO certification at what it describes as the strictest level available, and claims credentialing workflows run up to 10x faster than industry averages.
Key Features
● NCQA-certified PSV: Automated primary source verification against primary sources with full audit trails; Andros claims the strictest NCQA CVO certification level available
● Low-touch provider onboarding: Two out of three application processes auto-complete without requiring provider input; a robust data repository autofills provider information from verified sources
● Network development tools: Recruit, contract, credential, and monitor providers in one system; designed for organizations managing network adequacy and geographic coverage strategies
● Credentialing committee management: Andros can manage the full credentialing committee process on behalf of clients, including generating committee-ready files and managing approvals
● Flexible delivery and ongoing monitoring: Continuous monitoring with credentialing professionals following up on flagged discrepancies; outputs delivered via PDF download, web portal, or API for downstream integration
Pricing
Custom pricing based on organizational scope and volume. Contact Andros directly for a quote.
Pros
● One of the few platforms combining network development and credentialing in a single system
● NCQA-certified CVO with highly automated PSV and a large proprietary provider data repository
● Low-touch onboarding design minimizes provider input, reducing administrative friction at scale
Cons
- May be more complex than provider groups or growth-stage digital health companies need
- Less optimized for smaller provider groups needing individual payer enrollment execution
- Less established as a managed services execution partner for organizations that need end-to-end payer enrollment handled on their behalf.
4. CredentialStream
Best for: Hospital systems needing enterprise privileging, committee management, and EHR integration

CredentialStream is a credentialing platform from HealthStream designed primarily for hospitals and larger health systems with formal medical staff offices and established EHR systems.
It handles the full provider lifecycle within a single system, including application intake, primary source verification, reappointment, privileging, and provider enrollment. Everything sits under a single connected provider record, making it easier for teams to track status, manage approvals, and keep provider data organized.
One of its biggest strengths is integration. For health systems that need credentialing data to flow into platforms like Epic and other operational systems, CredentialStream can be a strong fit. That helps reduce duplicate data entry and keeps provider information more consistent across teams.
Key Features
- Provider lifecycle management: Handle end-to-end credentialing using patented technology
- Committee management: Automate workflows from application through committee review and approval
- EHR integration: Connect with Epic, Cerner, and Meditech via the hStream platform
- OPPE/FPPE: Integrate peer review data with credentialing for evidence-based privileging
Pricing
Subscription-based. Custom quotes based on organization size and the number of modules.
Pros
- Deepest privileging capabilities in the market
- Enterprise-grade reporting and audit trails
- Strong EHR integration ecosystem
Cons
- Steep learning curve and complex report building per users
- Higher price point suited to enterprise budgets
- Less suited for growth-stage digital health or smaller practices
5. Symplr Provider
Best for: Large multi-facility health systems needing credentialing within a broader GRC suite
Symplr (which acquired Cactus Software) is the legacy enterprise player in hospital credentialing. It integrates across the broader Symplr workforce management suite covering scheduling, compliance, and learning. For organizations already using Symplr products, the credentialing module connects naturally to existing workflows.
Key Features
- Credentialing and privileging: Manage the full provider lifecycle from application to performance monitoring
- Provider enrollment: Track enrollment with roster templates and payer-specific workflows
- OPPE/FPPE integration: Unify credentialing, privileging, and quality data
- DocuSign and reporting: Enable electronic signatures and custom reporting without coding
Pricing
Custom pricing based on organization size and the number of modules.
Pros
- Broadest GRC suite in the credentialing category
- Long track record with hospital systems
- Multi-function platform beyond credentialing
Cons
- Slow performance and inconsistent support quality
- Interface can feel cluttered with too many clicks for routine tasks
- Complex implementation
6. QGenda
Best for: Healthcare organizations needing credentialing natively connected to provider scheduling
QGenda is primarily a healthcare workforce scheduling platform. Its credentialing module exists as part of the broader ProviderCloud workforce suite. The defining differentiator is that credentialing status is natively integrated with scheduling. If a provider’s credential is about to expire, the scheduling system flags it. If a provider finishes credentialing, they become schedulable immediately without a manual handoff.
Key Features
- Credentialing-to-scheduling: Deploy providers the moment credentialing clears; expiring credentials flag the schedule
- Automated PSV: Run configurable verification workflows with audit trails
- OPPE/FPPE: Integrate practice evaluation with credentialing for evidence-based privileging
- Enterprise integrations: Connect with Epic, ADP, Workday, and other workforce systems
Pricing
Custom enterprise pricing based on organization size and the number of modules.
Pros
- Only platform connecting credentialing to scheduling in real time
- Strong user satisfaction
- Smooth onboarding experience with application pre-population
Cons
- Complex admin backend requiring significant implementation effort
- Enterprise pricing may be heavy for smaller organizations
- Some long-term users note recent changes to the customer support model
7. Incredable
Best for: Mid-market organizations and staffing firms needing highly configurable credentialing workflows
Incredable is a credentialing platform built by people who have worked in healthcare and know how messy credentialing can get in real life. One of the main things it leans into is flexibility. Teams can adjust workflows, forms, reporting fields, and payer tracking to match how they already work, instead of forcing everything into a rigid setup.
It covers the core pieces most teams care about, like document storage, expiration alerts, OIG and sanctions monitoring, payer enrollment tracking, license verification, task management, privileging, appointment workflows, and reporting.
Key Features
- Configurable workflows: Build custom credentialing workflows per payer, facility, or provider type
- AI-driven automation: Flag missing data, identify inconsistencies, and accelerate team decisions
- Exclusions monitoring: Screen across OIG, state licenses, and DEA registrations with automated notifications
- Provider app: Enable providers to upload documents, receive requests, and manage credentials from mobile
Pricing
Flat-fee model with no per-provider costs. Custom pricing upon request.
Pros
- Highly configurable; adapts to your workflows rather than forcing a fixed process
- User-friendly interface consistently praised in reviews
- Flat-fee pricing with no per-provider costs
- Responsive customer support and hands-on implementation
Cons
- Self-service model; your team still handles submission and follow-up
- Smaller market footprint than legacy players
8. Modio Health
Best for: Smaller practices needing an affordable, user-friendly system of record for credentials
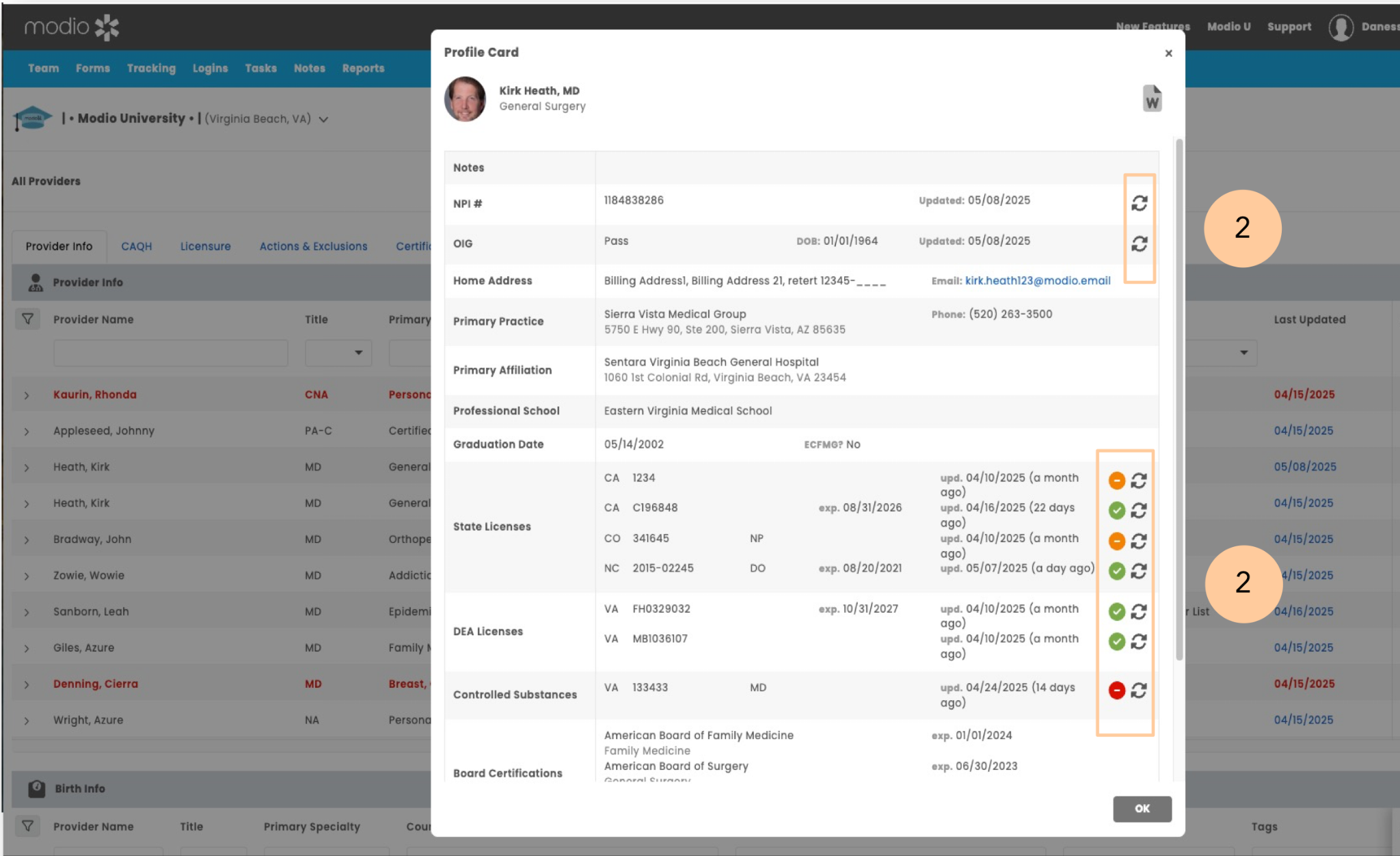
Modio Health OneView is a cloud-based credential management platform built by physicians and healthcare professionals. It is designed to give organizations a single place to store provider credentials, track expiration dates, and keep licensing information organized instead of searching through email threads, shared drives, or spreadsheets.
The platform focuses on credential lifecycle management. Teams can store documents, track license expirations, manage provider profiles, and monitor compliance tasks in a single system. OneView can also pull basic provider information from public registries like the NPI database to help pre-populate profiles and reduce manual data entry.
Where Modio works best is as a system of record for credentialing teams. Many organizations still perform the verification work themselves but use Modio to organize documents, track credentialing tasks, and manage provider records in one place.
Key Features
- Centralized credential storage: Store provider documents with expiration alerts and renewal reminders
- PSV data: Pull data from 100+ primary sources (manual trigger required)
- CME tracking: Track continuing medical education and generate provider CVs
- CAQH integration: Monitor CAQH profile status and re-attestation deadlines
Pricing
Custom pricing. Reviewers describe it as cost-effective relative to competitors.
Pros
- Highly user-friendly interface praised across review platforms
- Cost-effective for smaller practices
- SOC 2 Type 2 compliant data security
Cons
- No API available
- Verifications require manual clicks, not continuous background monitoring
- No licensing execution
How to Choose the Right Credentialing Software
Clarify what you need the platform to do. There is a real difference between a tool that stores credential data and one that submits applications, follows up with payers, and manages compliance. Knowing which category you need narrows the list immediately.
Plan for where you are headed, not just where you are. A platform that works at 20 providers in one state often falls apart at 100 providers across five states. If growth is part of the plan, factor in multi-state licensing and scalable enrollment in your decision.
Check for NCQA CVO certification. If delegated credentialing is on your roadmap, your vendor needs to be certified. Not every platform on this list qualifies.
Evaluate the support model. When a payer loses an application or changes a requirement mid-cycle, response time matters. Ask prospective vendors about SLA specifics: what they cover, what falls outside scope, and what happens when deadlines are missed.
Ask who is doing the work. Some platforms use in-house credentialing specialists. Others rely on offshore BPO teams. The difference shows up in first-pass rates and follow-up quality.
Still Deciding? Here's How We'd Narrow It Down
Choosing credentialing software comes down to one simple question. Do you want a system that only organizes your files, or one that actually moves credentialing forward?
Many platforms in this guide are solid, depending on what you need. Some are great for document management. Others fit large hospital systems with complex medical staff structures. But if your goal is to credential providers faster, reduce administrative work, and avoid revenue delays, the platform needs to do more than store data.
That is exactly what we built Assured for. If you want to see how fast modern credentialing can run, book a demo with Assured and we'll show you exactly how it works.
Frequently Asked Questions
What exactly does credentialing software do?
Credentialing software manages the verification of healthcare providers' qualifications (education, state licenses, board certifications, DEA registration, malpractice history, and sanctions status) against primary sources before they treat patients.
The best platforms also handle ongoing monitoring (so you know immediately if a license lapses or a sanction is posted), expirables tracking (proactive alerts before renewals are missed), and CAQH management (keeping the industry's standard data repository in sync). Credentialing software is distinct from payer enrollment software, which handles the separate process of submitting providers to insurance networks for reimbursement.
What is delegated credentialing, and why does it matter operationally?
Delegated credentialing is a formal arrangement in which a health plan accepts a physician group's credentialing decisions rather than running its own credentialing process for each provider. The operational impact is significant; instead of waiting months per provider per payer, a delegated group submits a roster, and the provider is recognized in-network. Achieving delegation requires typically 6 to 12 months of documented, NCQA-compliant credentialing history as a prerequisite.
The platform you're using today either builds that record or doesn't.
Do I need NCQA CVO certification in my credentialing vendor?
Not in every case. But if you're pursuing delegated credentialing, have health plan partners who audit your process, or need to demonstrate compliance to accrediting bodies, yes. "NCQA compliant" is self-declared. "NCQA CVO certified" is independently audited by NCQA against specific verification standards.
Among the platforms in this guide, Assured holds NCQA CVO certification.
What questions should I ask in a credentialing software demo?
Four that reveal the most:
(1) What is your documented first-pass approval rate, and how do you calculate it?
(2) Can we license the software without the managed service, and what does that look like?
(3) What is your current NCQA CVO certification status, and can I see the letter?
(4) Can you show me live how the platform handles an expired license or a flagged OIG result? A vendor that answers all four without hesitation is worth continuing to evaluate


.svg)
.png)



.svg)
.png)
.svg)
.png)
