Quick Summary
Every day a credentialed provider sits 'not yet enrolled, they lose revenue. Payer enrollment backlogs quietly cost digital health and multi-site groups millions a year. We put 8 automated enrollment tools based on submission speed, follow-up reliability, and whether their AI actually delivers in real workflows. Here are our top three picks:
What 'Automated Payer Enrollment' Actually Means
Most vendors call themselves "automated," but the label hides what's actually happening inside the platform. Here, automation means three very different things depending on the tool.
Some tools auto-populate payer application forms using data stored in the platform. That part is real and useful as it saves hours of manual data entry per application. But the tool stops there. Your team still logs into portals, uploads documents, submits, and chases follow-ups by phone and email.
A second tier uses bots and RPA to submit applications through payer portals. That moves further, but bots break when portals change. The monitoring and human escalation behind them is what actually determines whether applications go out clean.
The deepest end of automation is where AI handles the full lifecycle. It reads the payer's form, pulls data from CAQH, NPPES, and state boards, pre-validates every field, submits, follows up on cadence, and flags exceptions before they become rejections.
Why Listen to Us
We built Assured after scaling Dawn Health's provider network from 0 to 150+ providers across 15 states and dealing with every credentialing and enrollment bottleneck firsthand. Today, as an NCQA-certified CVO, we serve organizations nationwide. We know the workflows, the payer quirks, and what actually gets providers billing faster.

Side-by-Side Comparison of All 8 Tools
Here's how the 8 platforms compare at a glance before we get into each one in detail.
The 8 Best Automated Payer Enrollment Tools
1. Assured — AI-native payer enrollment built for organizations of all sizes and types
Best for: Organizations needing payer enrollment, credentialing, and licensing executed end-to-end
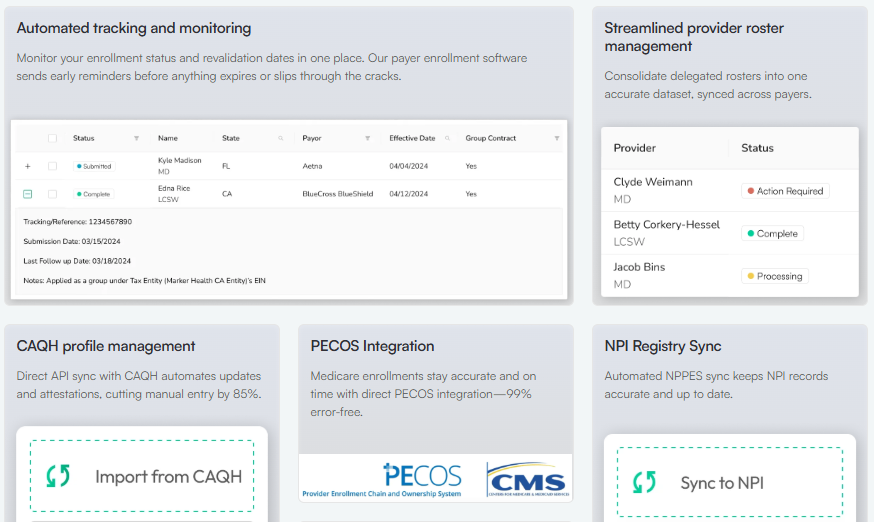
Assured is an AI-powered payer enrollment platform built for healthcare organizations that need to get providers in-network fast, stay continuously compliant, and scale without adding headcount. The platform automates the full enrollment workflow end-to-end.
We submit applications within 72 hours of receiving provider info, then follow up across payer portals on a fixed cadence until the provider is in-network. The AI reads each payer's specific application, auto-fills from CAQH, NPPES, DEA, and state board data, and runs pre-submission validation against payer rules that change week to week
These catch the issues that quietly kill first-pass approvals: closed panels, Optum's 5-TIN limit, telehealth-only licenses that Florida MA payers reject, and missing Medicaid credentials on D-SNP applications. Customers report 80–90%+ first-pass approvals as a result, with John Zhao, CEO of Blossom Health, calling the submission speed "something I don't think is true for other competitors."
See how Assured's AI handles a live payer enrollment, from CAQH pull to portal submission
Payer Enrollment Software Demo | Assured

Key Features
- AI form pre-fill: Reads payer-specific applications and auto-populates from CAQH, NPPES, and your provider roster
- Pre-submission validation: Catches data mismatches, closed panels, and specialty conflicts before the application goes out
- Automated follow-up: Tracks every submission across payer portals and follows up on a set cadence
- Real-time status dashboard: Full visibility into every application, no black-box BPO experience
- Integrated with credentialing + licensing: One platform, one data model, no handoffs between tools
- NCQA-certified CVO: Certified across all 11 verification elements for delegated credentialing support
Pros
- 72-hour submission SLA — among the fastest published in the category
- Pre-submission validation catches closed panels, CAQH gaps, and specialty/billing code mismatches before applications go out
- Active follow-up across payer portals on a set cadence until providers are in-network
- Direct W-2 fulfillment staff, not offshore BPO subcontractors
- Usage-based pricing that scales with provider volume, not per-seat headcount
Cons
- Newer to market than legacy incumbents
Pricing
Usage-based pricing that scales with provider volume. Custom quotes available on request.
2. Madaket Health — Enrollment-first platform with a 4,000+ payer library
Best for: Enterprise orgs and large networks needing breadth of payer coverage in a single system
Madaket Health is built around roster-level submissions and data-sharing agreements with major payers, which cuts redundant data entry across large provider bases enrolling across commercial, Medicare Advantage, and Medicaid MCO plans. It leans less on the AI-driven pre-validation layer newer entrants lead with, and more on scale and payer-network reach for networks managing enrollment at enterprise volume.
Key Features
- Broad payer network: Connections to 4,000+ payer organizations across commercial and government plans
- Roster submission: Bulk enrollment for provider groups sharing tax IDs
- Provider data management: Centralized profile and document management
- Payer directory updates: Push demographic changes to connected payers
Pros
- One of the largest payer-connection footprints in the category
- Strong fit for enterprise-scale enrollment volume
- Mature product with a long enterprise track record
Cons
- Less AI-driven pre-validation than newer platforms
- Interface reads as enterprise-legacy rather than modern SaaS
- Implementation can stretch over months for larger orgs
Pricing
Custom enterprise pricing; contact Madaket for a quote.
3. MedTrainer — AI form mapping plus credentialing in one suite
Best for: Clinics, FQHCs, and ambulatory surgery centers, bundling enrollment with compliance training and credentialing

MedTrainer packages credentialing, payer enrollment, compliance training, policy management, and incident reporting into one healthcare workforce compliance platform. AI form mapping auto-populates payer applications from a central provider record, though submission execution stays with your team.
Key Features
- AI-assisted form mapping: Auto-populates payer enrollment applications from the provider profile
- Credentialing workflows: Automated PSV, license tracking, and expirables monitoring
- Exclusion monitoring: Screens across OIG, LEIE, SAM, and 40+ databases
- Healthcare LMS: Hundreds of healthcare-specific training courses
Pros
- Only platform unifying credentialing, enrollment, LMS, and compliance
- Implementation runs 73% faster than the industry average, with customers live a month and a half sooner
- Support team answers 95% of calls within two rings
Cons
- Tracking program can be better for tracking product expiration dates
- Development team dependency can slow turnaround on requests and updates
- Not very intuitive
Pricing
Tiered subscription based on modules and access level.
4. Provider Passport — AI enrollment engine with RPA payer follow-ups
Best for: Health systems wanting AI-driven enrollment alongside credentialing, privileging, and provider data management

Provider Passport is an AI-first provider management platform covering payer enrollment, credentialing, privileging, and provider data management in one system. Its TruMation RPA layer handles portal submissions, uploads, and status polling without manual intervention.
Key Features
- Enrollment engine: AI-driven payer application filing tuned to roughly 4,500 payers
- TruMation RPA: Autonomous portal logins, form submissions, and status polls across mapped payers
- Integrated credentialing + privileging: Full provider lifecycle in one platform, not a point tool
- Provider data management: Real-time profiles pulled from 18+ sources, including state boards, DEA, and more
Pros
- AI-native architecture rather than automation retrofitted onto legacy software
- Credentialing, privileging, enrollment, and PDM in a single platform
- Deep payer coverage with specialty-specific logic
Cons
- Licensing management isn't part of the core scope
- Less established customer base than legacy incumbents
- RPA-heavy automation can require vendor updates when payer portals change
Pricing
Custom pricing upon request.
5. CredentialStream — Enterprise unified credentialing and enrollment
Best for: Hospital systems and academic medical centers needing enrollment integrated with privileging and EHR workflows

CredentialStream is HealthStream's enterprise credentialing and enrollment platform, built for hospitals and larger health systems with formal medical staff offices, established EHR systems, and committee-based privileging workflows. The enrollment module resides within a connected provider record that spans credentialing, privileging, reappointment, and PSV.
Key Features
- Unified provider record: Enrollment integrated with PSV, privileging, and reappointment
- Committee management: Routes enrollment and credentialing decisions through configurable approval workflows
- EHR integration: Connects with Epic and other major EHR and HRIS platforms via hStream
- HITRUST r2 certified: Highest standard of healthcare data security
Pros
- Deep enterprise footprint across large hospital systems
- Strong EHR integration ecosystem
- Enterprise-grade audit trails and reporting
Cons
- Steep learning curve and complex report-building per G2 reviews
- Pricing suited to enterprise budgets; not a fit for smaller practices
- Less agile than modern AI-first platforms for fast-growing digital health organizations
Pricing
Custom enterprise pricing upon request.
6. Modio Health — Clean interface for small-to-mid practice groups
Best for: Smaller practices and mid-sized groups wanting a user-friendly system of record for credentials and basic enrollment tracking
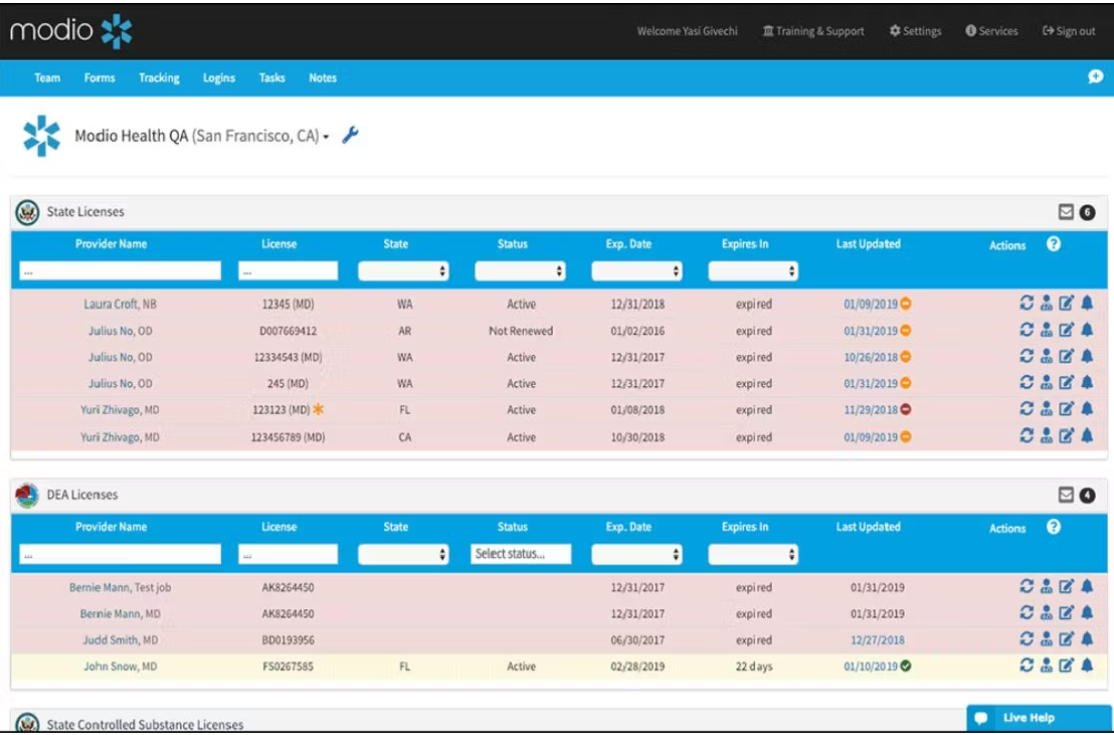
Modio Health's OneView is well-known in the credentialing-first category. On the payer enrollment side, it tracks status and stores applications along with credentialing documents, but it doesn't submit to or follow up with payers on your behalf. Teams typically use it as a warehouse for provider data, tracking enrollment progress within the platform while handling operational work outside it.
Key Features
- Centralized credential storage: Provider documents and expiration alerts in one place
- CAQH monitoring: Profile status and re-attestation tracking
- Manual PSV: Access to 100+ primary sources with on-demand verification triggers
- Enrollment tracking: Record enrollment status and documents, no submission engine
Pros
- Consistently praised for a user-friendly interface
- Cost-effective for smaller practices
- SOC 2 Type 2 certified
Cons
- No enrollment submission or follow-up automation
- No API available for system integration
- Manual verification triggers rather than continuous background monitoring
Pricing
Custom pricing.
7. CredentialingSpectrum — Auto-populated payer applications and contract management
Best for: Mid-market practices managing payer contracts alongside enrollment in one system
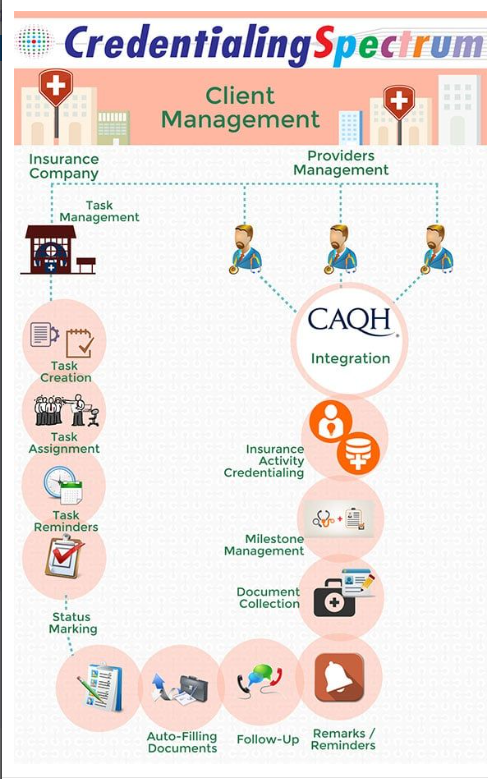
CredentialingSpectrum is a credentialing and payer enrollment platform built for mid-market practice groups. It auto-populates payer applications from stored provider data and layers in contract management, tracking effective dates, renewal timelines, and fee schedules alongside enrollment status.
Key Features
- Auto-populated applications: Fills payer forms from centralized provider data
- Contract management: Track effective dates, fee schedules, and renegotiation windows
- Credentialing workflows: Task tracking and document storage across credentialing and enrollment
- Expirables monitoring: Automated alerts for expiring licenses and contracts
Pros
- Contract management is a genuine differentiator in this category
- Mid-market pricing more accessible than enterprise platforms
- Focused feature set without the complexity of hospital-grade tooling
Cons
- Smaller market footprint than legacy incumbents
- Less AI-driven pre-validation than newer entrants
- Self-service model; execution stays with your team
Pricing
Custom pricing upon request.
8. Symplr Provider — Broad GRC suite with enrollment tracking
Best for: Large multi-facility health systems needing enrollment within a broader governance, risk, and compliance platform

Symplr, which acquired Cactus Software, is the legacy enterprise player in hospital credentialing and enrollment. Its provider module covers credentialing, privileging, payer enrollment tracking, and compliance monitoring, and integrates across the broader Symplr suite.
Key Features
- Provider enrollment tracking: Roster templates and payer-specific workflows
- Credentialing and privileging: Full provider lifecycle from application to performance monitoring
- OPPE/FPPE integration: Credentialing tied to quality and performance data
- DocuSign and reporting: Electronic signatures and custom reporting
Pros
- Broad GRC suite beyond just enrollment
- Long track record with hospital systems
- Multi-function platform for consolidated vendor strategy
Cons
- Users report slow performance and inconsistent support in G2 reviews
- Complex implementation timelines
- Interface can feel cluttered with too many clicks for routine enrollment tasks
Pricing
Custom enterprise pricing based on modules selected.
How to Choose the Right Payer Enrollment Tool?
1. If you're a digital health or multi-state outpatient org
Speed and multi-state execution are the two pressure points. Your enrollment vendor needs to submit within days, reliably follow up across dozens of payers per state, and handle virtual addresses and payer-specific telehealth rules. Look for platforms with published submission SLAs, sub-24-hour support, and NCQA-certified CVO status. Digital health operators tend to outgrow self-service tools quickly.
2. If you're an enterprise health system
Integration is the first screen. Your enrollment platform needs to flow data into the EHR, work with delegated credentialing arrangements, and support roster-level submissions across multiple tax entities. CredentialStream and Symplr Provider are the usual shortlist.
However, if submission speed and AI depth are priorities, Assured is worth evaluating first. Unlike legacy platforms, Assured initiates payer enrollment submissions within 72 hours, automates CAQH management, and handles credentialing, licensing, and monitoring in one system
3. If you're a small practice or group
Prioritize ease of use and cost-efficiency. If your organization is primarily looking for a compliance or LMS-adjacent solution, Modio Health, MedTrainer, and CredentialingSpectrum are worth evaluating. That said, if credentialing speed, payor enrollment, and multi-state licensing are part of the requirement, Assured deserves a look.
Still on the Fence? Here's How We'd Sum It Up
Most of the tools on this list handle the basics of payer enrollment. The meaningful differences show up in how fast they actually submit, how reliably they follow up, and whether the AI holds up in real workflows.
If you want enrollment applications out the door in 72 hours, ~95%+ first-pass approval rates that compress time-to-revenue, and an NCQA-certified CVO behind every file, book a demo with Assured, and we'll show you exactly how it works.
FAQs
1. How is payer enrollment different from credentialing?
Credentialing verifies the provider, their education, licenses, board certifications, DEA, NPDB record, and sanctions status. Payer enrollment verifies that the provider is in-network with insurance carriers so the organization can bill for their services.
2. How long does automated payer enrollment actually take?
Submissions happen within days on modern platforms. Industry standard is 90 to 120 business days; Assured submits within 72 hours and conducts follow-ups throughout the entire approval window.
3. Can payer enrollment be fully automated end-to-end?
Not entirely. Submission, CAQH management, application auto-fill, and follow-up tracking can all be automated but payer approval can't. Once an application is in a payer's queue, no software controls how fast it moves. The best platforms compress everything on the submission side and follow up proactively on the rest.
4. Do these tools handle Medicare Advantage and Medicaid enrollment?
Most do, though coverage varies by plan and state. Medicare enrollment specifically has its own workflow (PECOS, MAC regions, revalidations) that not every platform handles with equal depth. However, Assured handles both, with payer-specific application logic, portal automation, and real-time status tracking.
5. How do these tools handle payer panel closures?
The better platforms detect closures before you submit and flag them during pre-validation. Others submit anyway, and you find out weeks later when the denial comes back. Assured's pre-submission validation specifically checks for closed panels, incomplete documentation, and specialty conflicts before any application goes out, which is a core reason first-pass approval rates run at ~95%+
6. How much does payer enrollment software cost?
Ranges from a few thousand a month for smaller practice-focused tools to enterprise contracts well into six figures annually. Usage-based pricing tends to align cost with growth; fixed per-seat or per-application pricing penalizes scale.



.png)




.png)

